Iron deficiency is the most common micronutrient deficiency in the world. In contrast to most other nutrient deficiencies, iron deficiency is widespread in both developing countries and in more developed nations such as Ireland. Although widespread from a geographical standpoint, the risk of deficiency is greatest amongst only part of the population in any country, namely women and young children.

Written by Dr Elaine McCarthyLecturer in Nutrition at the School of Food and Nutritional Sciences in University College Cork (UCC) and Lead Investigator at UCC’s internationally renowned INFANT Research Centre
Iron is essential for the transport of oxygen (and carbon dioxide) around the body due to the critical role it plays in haemoglobin and red blood cell development. Aside from this key function, iron is critical to most cells and organ systems as it is an essential component of many proteins and enzymes, especially those involved in energy metabolism.
Iron deficiency should be considered along a continuum. The earliest stage is classified as iron depletion, due to a reduction in iron stores in the body, that are mostly in the form of the storage protein ferritin. This depletion can progress into iron deficiency, where reductions in iron transport proteins such as transferrin are also seen. Prolonged depletion and deficiency will lead to iron deficiency anaemia (IDA), characterised by a reduction in the functional capacity of the body, presenting as reduced haemoglobin concentrations.
Symptoms of iron depletion or deficiency are not always apparent as the body uses its iron stores to protect erythropoiesis and haemoglobin production. However, symptoms of a more prolonged deficiency, resulting in IDA can include tiredness, weakness, dizziness, gastrointestinal (GI) upset, reduced immune function, a lack of energy and difficulties with concentration.
Most recent estimates suggest that iron deficiency anaemia affects over 1.2 billion people worldwide. It is considered one of the leading contributors to the global burden of disease, but particularly amongst premenopausal women and young children.
Anaemia is even more common, estimated to affect one third of the global population but iron deficiency is only one such cause of anaemia. This is important to remember, as there are many other nutritional and non-nutritional causes of anaemia so appropriate testing and diagnosis are essential.
Risk factors for iron deficiency
There are three underlying causes of iron deficiency and IDA: an inadequate iron uptake, elevated blood losses and/or increased iron requirements.
Issues with iron uptake can be due to a diet lacking in ironrich foods and/or an inability to absorb dietary iron, as is the case in conditions characterised by malabsorption. Inadequate dietary iron intakes have been frequently reported in the Irish population but most commonly amongst toddlers, school-age children and adult women. Individuals following a vegetarian or vegan diet can be at particular risk of poor dietary iron intakes, especially of the highly bioavailable haem iron.
Increased blood losses occur most frequently through menstruation in women of reproductive age. Iron losses during menstruation vary significantly amongst women but a woman typically loses at least 1 mg of iron per cycle or roughly 0.3-0.6 mg of iron per day. Women with heavy or prolonged periods can lose 5-6 times this amount of iron, further increasing their risk of deficiency.
Chronic blood losses from the digestive tract can also put an individual at risk of iron deficiency. While iron deficiency and IDA are considered uncommon amongst men, GI bleeding caused by inflammatory bowel disease, ulcers or certain cancers is an important risk factor to consider in this cohort.
Due to the critical role of iron in almost all bodily functions, requirements for iron increase dramatically during periods of rapid growth and development. These key periods of life include pregnancy, lactation, infancy and early childhood.
Iron requirements increase almost 10-fold during pregnancy, with the greatest demand seen during the third trimester to support the needs of both the mother and her growing child. While the body can make remarkable adaptations during pregnancy to increase the rates of iron absorption from the diet, meeting these high requirements remain a challenge for many pregnant women.
Rates of iron deficiency in pregnant women across Europe range from 28% to as high as 85% in some parts. Poor dietary iron intakes and compliance with dietary guidelines are widely reported in this population.
Perhaps more troublesome again is that European data suggests that almost half of women are iron depleted prior to ever becoming pregnant. The stark reality is that, physiologically, many women are on the back foot in terms of iron levels long before they ever become mothers.
In addition to the unwanted symptoms of tiredness and weakness, IDA during pregnancy can result in adverse pregnancy outcomes including preterm birth and a low-birth-weight baby. Further to this, it also increases the chances that the baby itself will be born iron deficient.
This is important as iron plays a fundamental role in the growth and development of a child’s brain, most of which occurs in the first 1,000 days i.e. during the pregnancy and first 2 years of a child’s life. Iron deficiency during this critical period of development can result in poorer intelligence, low cognition, poor motor skills and behavioural problems that are often long-lasting.
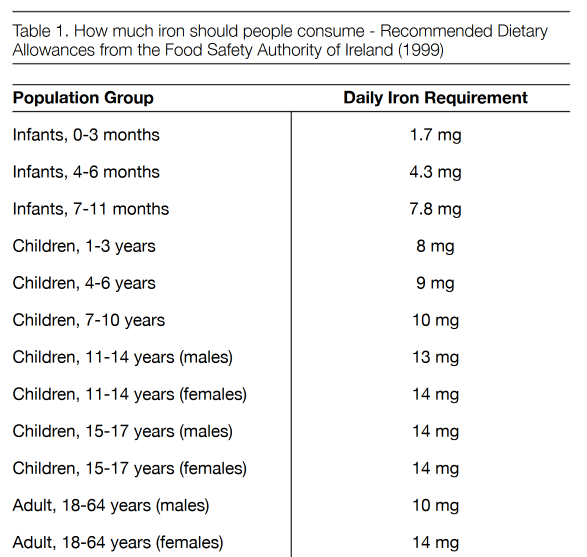
A functional iron deficiency?
Perhaps less considered or acknowledged is something termed a functional iron deficiency. A functional deficiency can occur despite adequate dietary iron intakes or large stores of iron in the body. However, the use and/ or uptake of this iron is impeded, typically through the action of the iron regulatory hormone, hepcidin. During times of inflammation, hepcidin concentrations are elevated which prevents the body from absorbing iron. While inflammation is commonplace in certain disease states, this phenomenon has also been reported in more low-grade, chronic inflammation such as that seen during obesity. This effect is seen in the pregnant population too, with maternal obesity both prior to and during pregnancy associated with an increased risk of iron deficiency in the mother and her newborn baby.
This type of functional deficiency or inflammatory induced deficiency has most recently been acknowledged in athletes and physically active individuals. This inflammatory effect, coupled with increased iron losses particularly via higher rates of sweating and GI bleeding, puts athletes and other physically active individuals at risk for iron deficiency.

Strategies to combat the problem
When it comes to iron, the saying “too much of a good thing” rings true. Excess iron is toxic and extremely harmful to the body; therefore, appropriate testing and diagnosis are critical first steps. Once a diagnosis of iron deficiency or IDA is confirmed, the aim of treatment is to replenish iron stores and if anaemia is present, return haemoglobin concentrations to normal. The first line of treatment involves oral iron supplements, typically in the form of ferrous sulfate, gluconate or fumarate. Multivitamin-mineral preparations usually contain too low a dose of iron to correct a deficiency and may contain other minerals, such as zinc, that can inhibit iron absorption. Iron supplements are available in tablet or liquid form, with controlled or slow-release preparations possible.
Previous treatment guidelines proposed a daily dose of 100200 mg elemental iron divided into multiple doses across the day. Following advancements, particularly in our understanding of hepcidin and its control over iron absorption, many recent guidelines recommend lower doses (30-60 mg) once daily or even intermittently, every second day. Intermittent supplementation has been shown to be effective in improving iron status but with fewer side effects. Improvements in haemoglobin concentrations should be seen within weeks of effective iron treatment, but it may take 3-6 months of treatment for a complete replenishment of iron stores.
While this form of treatment is effective, compliance with such supplementation strategies is extremely poor in the population.
GI side-effects are widely reported, in up to 75% of users in some studies, and include diarrhoea, constipation, abdominal pain, nausea, flatulence and black stools. A deleterious effect of oral iron supplementation on the gut microbiota has also been proposed. Recent advances in the incorporation of ferrous iron into whey protein microspheres has shown promise for protection against these side effects.
Alongside any supplementation strategy, the importance of an individual’s daily diet should not be ignored. The absorption of iron is highly influenced by a series of promotors and inhibitors in the diet, so the following advice should be remembered:
• Oral iron supplements are most effective when taken on an empty stomach or at least an hour before meals, and preferably in the morning.
• Iron supplements shouldn’t be taken with milk, antacids or calcium supplements.
• Iron absorption is strongly inhibited by the phytic acid found in whole grains and pulses and the polyphenols found in coffee, teas and chocolate. So avoid that cuppa while taking your supplement!
• Vitamin C or ascorbic acid is a very potent enhancer of iron absorption. If people find it difficult to take supplements on an empty stomach and need to take it with a small meal, including a good source of vitamin C with the meal can help to overcome the inhibitory effect of the meal.
• Don’t forget that many foods are good natural sources of iron or have been fortified with iron, including lean meat and poultry, beans and pulses, nuts and dried fruit, fortified breads and cereals.
View the February Magazine here